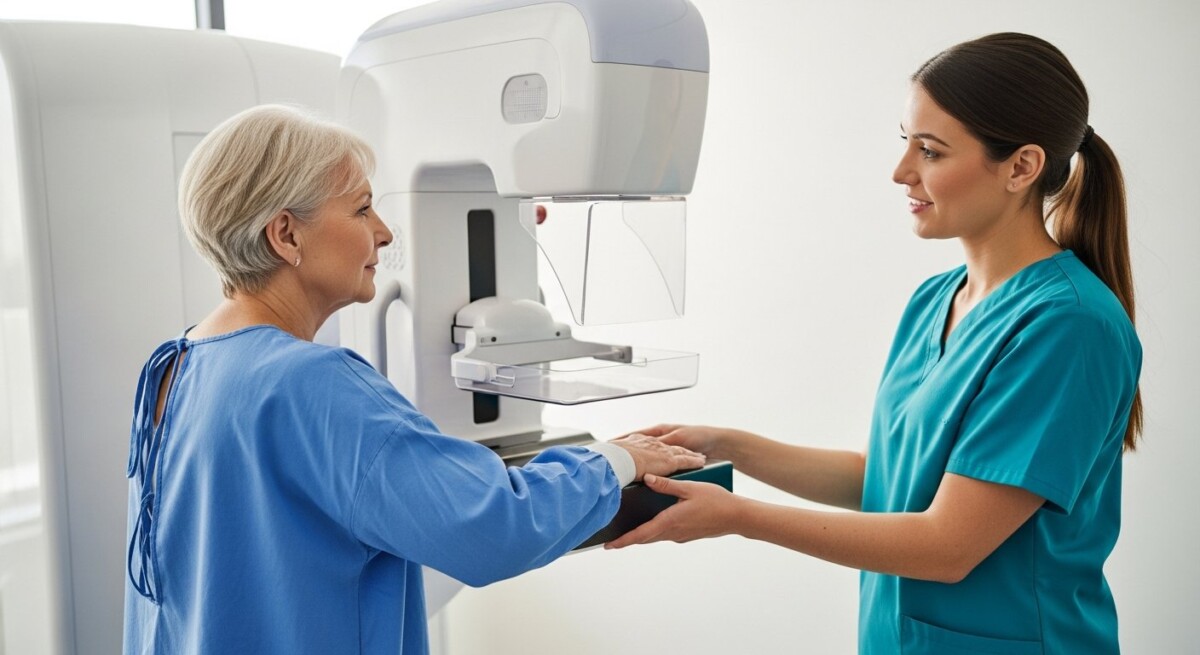
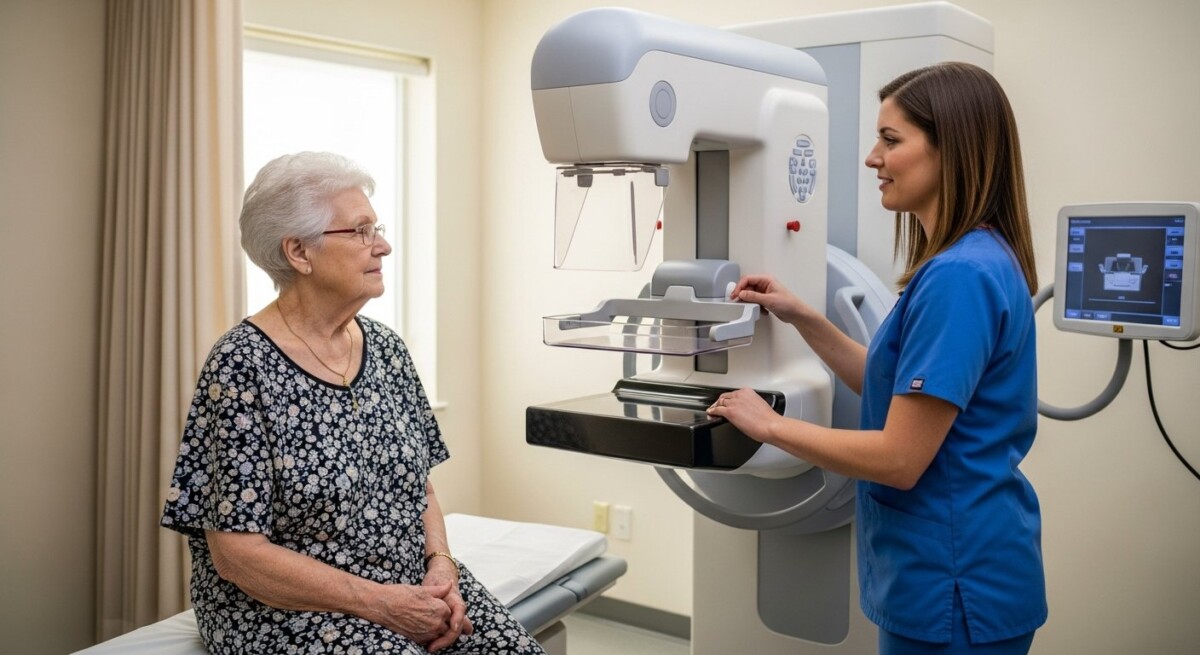
Medicare Mammogram Coverage After 70: Your Guide to Frequency
For millions of American women aged 70 and older, maintaining breast health remains a vital priority. A common and pressing question arises: how often does Medicare pay for mammograms after age 70? The answer is not just a simple date on a calendar, but a nuanced policy rooted in clinical guidelines and personal health history. Understanding the specifics of Medicare coverage for these essential screenings can empower you to make informed decisions about your preventive care without unexpected financial burden. This comprehensive guide will detail the official coverage rules, explain the critical factors that influence screening frequency, and provide practical steps to ensure you receive the benefits to which you are entitled.
Medicare’s Official Coverage Policy for Mammograms
Medicare Part B (Medical Insurance) provides coverage for screening mammograms to help detect breast cancer early, when it is most treatable. The coverage rules are clearly defined by the Centers for Medicare & Medicaid Services (CMS). For all women with Medicare who are age 40 and older, a screening mammogram is covered once every 12 months. This annual benefit does not have an upper age limit. Therefore, the direct answer to how often Medicare pays for mammograms after age 70 is: once every calendar year. There is no automatic cutoff at age 70, 75, or any other age. Your eligibility for this annual preventive service continues as long as you are enrolled in Medicare Part B.
It is crucial to distinguish between a screening mammogram and a diagnostic mammogram. A screening mammogram is a routine check for women who have no signs or symptoms of breast disease. This is the service covered annually. A diagnostic mammogram is a more detailed X-ray used to investigate a specific breast concern, such as a lump, pain, nipple discharge, or an abnormal finding from a screening mammogram. Diagnostic mammograms are covered by Medicare Part B as well, but they are subject to different cost-sharing rules. While screening mammograms often have $0 cost-sharing if your doctor accepts assignment, diagnostic mammograms typically involve paying 20% of the Medicare-approved amount after you meet your Part B deductible.
Factors Influencing Your Personal Screening Schedule
While Medicare provides the financial framework for an annual mammogram, your personal screening schedule should be a collaborative decision made with your healthcare provider. The “once per year” coverage is a maximum frequency from Medicare’s perspective, not a mandated schedule. Several key factors will influence whether an annual mammogram is the right choice for you after age 70.
Your overall health and life expectancy are primary considerations. The goal of cancer screening is to detect disease at a stage where treatment can improve longevity and quality of life. Healthcare providers often use guidelines from organizations like the U.S. Preventive Services Task Force (USPSTF), which recommends biennial screening for women aged 70 to 74 and states evidence is insufficient for women 75 and older. However, other groups, like the American Cancer Society, emphasize continuing screening as long as a woman is in good health and has a life expectancy of 10 years or more. This personalized approach is essential. A woman aged 72 in excellent health may benefit more from annual screening than a woman aged 78 with multiple chronic, life-limiting conditions.
Your personal and family history of breast cancer dramatically impacts screening recommendations. Women with a personal history of breast cancer, a genetic mutation (like BRCA1 or BRCA2), or a very strong family history are typically advised to continue more frequent screening, which may include annual mammograms and sometimes supplemental imaging like breast MRI. Dense breast tissue is another significant factor. Women with dense breasts have a higher risk of breast cancer, and mammograms can be less effective in detecting tumors in dense tissue. In these cases, your doctor may recommend annual screening or additional tests. Understanding your own risk profile is a critical part of the conversation with your doctor when deciding on screening frequency.
Costs and Coverage Details You Need to Know
For most beneficiaries, the out-of-pocket cost for a Medicare-covered screening mammogram is $0. This is true if your doctor or imaging center accepts Medicare assignment. This means they agree to accept the Medicare-approved amount as full payment. You pay nothing for the mammogram itself, and the Part B deductible does not apply. This makes preventive care highly accessible. However, there are important scenarios where you could incur costs.
If you have a diagnostic mammogram, you will be responsible for 20% of the Medicare-approved amount, and the Part B deductible applies. Furthermore, if you choose a facility that does not accept assignment, they can charge you up to 15% more than the Medicare-approved amount (known as an excess charge). It is always wise to confirm that the facility and radiologist accept Medicare assignment before your appointment. If you are enrolled in a Medicare Advantage Plan (Part C), your plan must cover at least the same level of benefits as Original Medicare (Part A and Part B), but it may have different rules for networks, referrals, and cost-sharing. Always check with your specific plan to understand your coverage details and any associated copayments.
Medicare also covers newer digital breast tomosynthesis, often called 3D mammography, under the same guidelines. If the facility offers both 2D and 3D mammography and you receive a 3D mammogram, Medicare will cover it as a screening mammogram. There should be no additional cost to you if the provider accepts assignment. For women at high risk, Medicare Part B also covers one baseline mammogram for women aged 35-39 and covers a clinical breast exam as part of the pelvic exam (which includes a Pap test) once every 24 months, or every 12 months for certain high-risk individuals. For a deeper look at coverage nuances as you age, our resource on Age Defying Care: Exploring Medicare’s Mammogram Coverage After 75 provides extended insight.
How to Access Your Medicare Mammogram Benefit
Accessing your annual mammogram benefit is a straightforward process, but following the correct steps ensures smooth billing and no surprise bills. First, schedule your appointment with a clinic, hospital, or imaging center that accepts Medicare. When you call, you can explicitly ask, “Do you accept Medicare assignment for screening mammograms?” This confirms your $0 cost-share. You do not need a referral from your primary care physician for a screening mammogram if you are seeing a doctor who accepts Medicare. However, some imaging centers may require a doctor’s order, so it’s best to check when scheduling.
When you arrive for your appointment, have your red, white, and blue Medicare card or your Medicare Advantage Plan card ready. The facility will handle the billing directly with Medicare. You should receive a Medicare Summary Notice (MSN) or an Explanation of Benefits (EOB) from your Medicare Advantage Plan in the mail afterwards. Review this document carefully. It is not a bill, but it shows what services were billed, what Medicare paid, and what you owe. If the notice shows you owe money for a screening mammogram, contact the provider first to ensure it was billed with the correct diagnostic code. As with any Medicare service, keeping detailed records of your preventive care visits is wise. For more on navigating Medicare’s coverage rules for other specific procedures, you can reference our analysis on whether Medicare pays for tooth extractions.
To maximize your benefits and health, consider these key action steps:
- Discuss breast cancer screening annually with your primary care physician or gynecologist during your Medicare Annual Wellness Visit.
- Bring your personal and family health history to the conversation to inform a shared decision.
- Mark your calendar to schedule your mammogram 11 full months after your last one to utilize the full annual benefit.
- Always verify that the imaging center and radiologist accept Medicare assignment before your appointment.
- Keep copies of your mammogram reports and share them with all your healthcare providers.
Frequently Asked Questions
Q: Does Medicare cover mammograms after age 80?
A>Yes, Medicare Part B covers a screening mammogram every 12 months for beneficiaries with no age limit. The decision to continue screening should be based on an individual’s health status and life expectancy, in consultation with their doctor.
Q: I had a diagnostic mammogram last year. Does that use up my annual screening benefit?
A>No. Diagnostic and screening mammograms are billed differently. Having a diagnostic mammogram does not prevent you from getting your annual screening mammogram in the same calendar year. You are entitled to both if medically necessary.
Q: What if my doctor recommends a mammogram more than once a year?
A>If there is a medical reason, such as monitoring a previously found abnormality, Medicare will cover additional mammograms as diagnostic services. You would be responsible for 20% of the cost after your Part B deductible.
Q: Are 3D mammograms covered?
A>Yes, Medicare covers digital breast tomosynthesis (3D mammography) as a screening tool. If performed at a facility that accepts assignment, you should have no out-of-pocket cost for the 3D mammogram itself.
Q: Does Medicare cover other breast cancer screenings, like MRI or ultrasound?
A>Medicare may cover breast MRI or ultrasound as a diagnostic tool for women at high risk or to investigate an abnormal finding. Coverage requires meeting specific criteria and involves cost-sharing. For complex financial planning around healthcare, our section on Legal Health Finance offers broader guidance.
Navigating Medicare coverage for preventive services like mammograms is a key component of managing your health in later years. By understanding that Medicare pays for a screening mammogram once every 12 months after age 70 without an age cutoff, you can confidently plan your preventive care. The most important step is to engage in an ongoing, informed dialogue with your healthcare provider. Together, you can weigh your personal health history, risk factors, and overall well-being to determine the screening frequency that is right for you. This proactive approach, supported by Medicare’s annual benefit, empowers you to prioritize your breast health as part of a comprehensive wellness strategy throughout your senior years. Remember, staying informed about all your benefits, including those for Durable Medical Equipment, helps ensure you receive the full spectrum of care you’ve earned.